Seasonal allergies, also known as hay fever or pollen allergies, are usually linked to sneezing, itchy eyes, and runny noses. But many people don’t realize that these allergies can also affect the skin. When pollen comes into contact with your body, your immune system may overreact, releasing chemicals like histamine. This doesn’t just cause nasal congestion—it can also lead to rashes, redness, and itchy patches on the skin.
Here’s why seasonal allergies are more than just a breathing problem:
- Skin as the first barrier: Your skin comes into direct contact with pollen floating in the air, which can irritate or trigger a rash.
- Immune system reaction: When your body sees pollen as a threat, it releases histamine that can cause skin inflammation.
- Worsening existing conditions: People with eczema, asthma, or sensitive skin are more likely to develop allergy-related rashes.
- Areas most affected: The face, neck, arms, and chest are the most common sites for pollen-related skin irritation.
2. Recognizing the Appearance of Pollen Allergy Rash
Pollen allergies don’t look the same for everyone. Some people only experience mild redness, while others may develop more noticeable rashes or hives. Knowing what a pollen rash looks like helps you separate it from acne, heat rash, or other skin issues.
Here are the most common ways pollen allergy rash shows up on the skin:
- Eczema-like patches (Atopic Dermatitis):
- Dry, red, flaky, and itchy skin.
- May crack or ooze if scratched too much.
- Often worsens during pollen season if you already have eczema.
- Hives (Urticaria):
- Raised, red welts that are very itchy.
- Turn white in the center when pressed.
- Appear suddenly and may fade within hours but can return repeatedly
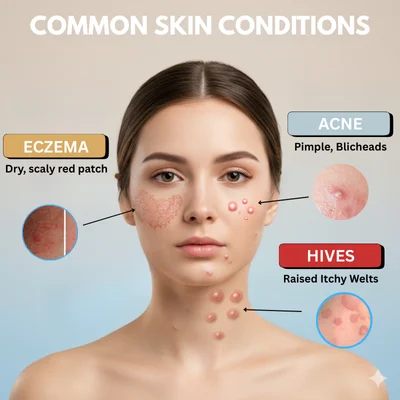
- Commonly affected areas:
- Face and neck → frequent exposure to airborne pollen.
- Arms and chest → pollen sticks to clothing and irritates exposed skin.
- Differences from acne or irritation:
- Allergy rashes are usually itchy, while acne is more tender or painful.
- Hives appear quickly and vanish, while acne develops gradually.
Key takeaway: If your rash comes and goes with pollen season, feels itchy, and worsens outdoors, it’s likely linked to a pollen allergy.
3. Why Seasonal Allergies Trigger Itchy Rashes and Hives

When pollen fills the air, it doesn’t just irritate your nose and eyes—it can also upset your skin. The body treats pollen like a harmful invader, and this triggers a chain reaction that leads to redness, swelling, and itching.
Here’s how it works step by step:
- Pollen enters the body:
- Through breathing → irritates nose, lungs, throat.
- Through skin contact → settles on exposed areas like the face, neck, and arms.
- Immune system overreaction:
- The body mistakes pollen for a dangerous substance.
- It releases histamine, a chemical responsible for itching, swelling, and rashes.
- Skin response to histamine:
- Blood vessels widen, making skin red and inflamed.
- Nerve endings become irritated, causing intense itching.
Fluid leaks into skin tissues, forming hives or welts.
- Risk factors that make rashes worse:
- Pre-existing eczema or sensitive skin.
- Family history of asthma or allergies.
- Wearing pollen-covered clothes for long periods.
- Exposure to other triggers like dust mites, mold, or pet dander.
4. Stages of an Allergic Reaction You Should Know
Allergic reactions often unfold in different stages, ranging from mild irritation to dangerous medical emergencies. By understanding each stage, you can recognize how your body is responding and take the right action at the right time.
The First Stage: Sensitization Without Symptoms
The process begins the first time your body encounters pollen or another allergen. Even though pollen itself is harmless, your immune system mistakes it for a threat and creates special antibodies to fight it. This stage is called sensitization. You may not feel any symptoms yet, but your immune system is now primed to overreact the next time you are exposed.
The Second Stage: Early Symptoms on Skin and Airways
During repeated exposure, the immune system releases histamine, the chemical that drives most allergy symptoms. This is when you may notice sneezing, nasal congestion, watery eyes, and itching. On the skin, it often appears as mild redness, small bumps, or dry, irritated patches. At this stage, the reaction is uncomfortable but usually manageable with simple home remedies or over-the-counter medications.
The Third Stage: Worsening and Spreading Symptoms
If pollen exposure continues, the reaction can intensify. Skin irritation may spread, hives become more noticeable, and eczema patches feel drier and itchier. Some people also report fatigue, headaches, and throat discomfort as their immune system continues to fight. This stage is often when seasonal allergy rashes become most visible, making the skin feel hot, itchy, and inflamed.
The Fourth Stage: Severe Swelling and Breathing Issues
In some cases, allergic reactions move beyond surface irritation and affect deeper tissues. This stage is called angioedema. The lips, eyelids, and face may swell significantly, and the swelling can extend to the throat. Breathing may become difficult, with wheezing or chest tightness. This is a warning sign that the allergy is becoming serious, and medical care is needed.
The Fifth Stage: Anaphylaxis as a Medical Emergency
The most severe stage of an allergic reaction is anaphylaxis. This is a life-threatening emergency where swelling blocks the airways, blood pressure drops suddenly, and breathing becomes extremely difficult. People experiencing anaphylaxis may feel faint, develop a weak pulse, or even lose consciousness. Immediate treatment with epinephrine and urgent medical care is essential to prevent fatal outcomes.
Understanding the Bigger Picture
Most people with pollen allergies never go beyond the second or third stage, experiencing only rashes, hives, and mild skin irritation. Still, being aware of all five stages ensures you can identify when a normal allergy becomes a medical emergency. Early recognition is the best protection.
5. Secondary Symptoms Linked With Pollen Allergies
Seasonal allergies don’t always stop at rashes, sneezing, and watery eyes. In some cases, the immune system’s overreaction can trigger symptoms that seem unrelated at first glance. These secondary issues are less common but still important to recognize.
Dry Mouth and Dehydration
When nasal congestion forces you to breathe through your mouth, it can quickly dry out your throat. Some antihistamines also reduce saliva, making the dryness worse.
Back Pain and Body Aches
- Inflammation caused by allergies may add stress to muscles and joints.
- Constant coughing and sneezing can strain the back and shoulders.
Dizziness and Lightheadedness
- Pollen allergies may affect the inner ear, leading to balance problems.
- Low blood pressure during stronger allergic reactions can also cause dizziness.
Itchy Scalp and Skin Irritation
- Pollen often settles on the scalp and hair outdoors.
- This can make your head feel itchy and uncomfortable, especially if you sweat.
These secondary symptoms don’t happen to everyone, but they can make allergy season much harder to deal with. Managing the root allergy usually helps reduce these additional discomforts.
6. Knowing When to See a Doctor or Allergist
Most pollen-related rashes and allergy symptoms are mild and manageable with home care. However, some situations require professional help. Knowing when to visit a doctor can prevent symptoms from getting worse and help you find the right treatment.
Mild Symptoms – Manage at Home
- Small, itchy rashes that fade within a few days.
- Occasional sneezing, watery eyes, or mild hives.
- Relief with over-the-counter antihistamines or creams.
When to See a Doctor
- Rash lasts more than a week or keeps coming back.
- Swelling around the eyes, lips, or face that does not settle.
- Symptoms interfere with sleep, work, or daily activities.
- OTC medicines are no longer effective.
When to Seek Emergency Care
- Sudden swelling of the tongue, throat, or lips.
- Difficulty breathing, wheezing, or chest tightness.
- Feeling dizzy, faint, or noticing a rapid drop in blood pressure.
Start with your primary care doctor for most allergy concerns. If symptoms are severe or you need testing, they may refer you to an allergist, who specializes in diagnosing and treating allergies.
7. Treatment Options for Allergy-Related Skin Rashes
Skin rashes from pollen allergies can be managed with the right mix of medicines, home remedies, and lifestyle care. The treatment you need depends on whether your symptoms are mild, persistent, or severe.
Over-the-Counter Relief for Mild Rashes
For quick comfort, antihistamines such as cetirizine or loratadine reduce itching and swelling by blocking histamine. Hydrocortisone creams or soothing lotions like calamine help calm red, inflamed skin. If pollen irritates your eyes, antihistamine eye drops can ease the itching and watering.
Prescription Medications for Stronger Symptoms
When store-bought medicines aren’t enough, doctors may recommend stronger corticosteroid creams for eczema patches, leukotriene inhibitors like montelukast for inflammation, or prescription-strength antihistamines for recurring hives. These treatments provide stronger control when flare-ups don’t settle with basic care.
Immunotherapy for Long-Term Allergy Control
For severe or year-round pollen allergies, immunotherapy—through allergy shots or under-the-tongue tablets—can retrain the immune system to react less strongly to pollen. Although this process takes time, it offers lasting relief and helps reduce the frequency of rashes and other symptoms.
Home Remedies That Calm Irritated Skin
At home, simple methods can bring soothing relief. A cold compress reduces swelling and itching, while oatmeal or baking soda baths calm irritated skin. Regular moisturizing with fragrance-free creams that contain ceramides or hyaluronic acid strengthens the skin barrier and prevents flare-ups.
Skincare Habits That Prevent Flare-Ups
Daily routines matter as much as medicines. Avoid hot showers, harsh soaps, and heavily fragranced products that strip or irritate the skin. Choose lukewarm showers, moisturize immediately afterward, and wear loose, breathable clothing so sweat doesn’t make rashes worse.
Combining Treatments for Best Results
Most people benefit from using a mix of medical treatment, home remedies, and preventive care. Finding the right balance helps control rashes quickly and reduces the risk of flare-ups during high pollen season.
8. Simple Prevention Tips to Reduce Pollen Rash

The most effective way to deal with allergy rashes is to limit pollen exposure. While avoiding it completely isn’t possible, smart habits can keep symptoms under control.
Check Pollen Counts Before Going Out
Weather apps and allergy forecasts show daily pollen levels. Plan outdoor activities when levels are lower, usually after rainfall or in the evening.
Keep Windows Closed During Allergy Season
Open windows allow pollen inside. Use air conditioning with clean filters or install HEPA air purifiers to keep indoor air safer.
Protect Your Face and Skin Outdoors
Wear sunglasses, a hat, and even a light mask to shield your face from pollen. A thin layer of petroleum jelly around your nostrils can trap pollen before it enters.
Clean Up Quickly After Outdoor Exposure
Shower and wash your hair after spending time outside to remove pollen particles. Change into clean clothes immediately instead of wearing pollen-covered ones indoors.
Strengthen Your Skin With Proper Care
Moisturize daily with fragrance-free creams to build a healthy skin barrier. Avoid harsh cleansers that strip natural oils, since dry skin reacts more easily to allergens.
Small Habits That Make a Big Difference
Simple actions like rinsing your face during the day, keeping bedding clean, and staying hydrated help reduce irritation and keep your skin calmer during pollen season.
9. Quick Answers to Common Allergy Rash Questions
Can seasonal allergies cause hives?
Yes. Pollen can trigger the release of histamine, which causes hives (urticaria)—raised, red, itchy bumps that often appear suddenly and fade within hours.
How long can an allergy rash last?
- Mild hives may disappear in a few hours.
- Eczema flare-ups can last days to weeks if untreated.
- If a rash lingers longer than 2 weeks, see a doctor.
Is coughing a sign of an allergic reaction?
- Yes, especially when pollen irritates the throat or airways.
- Allergic coughing is usually dry, unlike the wet cough of a cold.
- Persistent coughing with wheezing or shortness of breath requires medical attention.
Can pollen allergy cause dizziness?
- Dizziness may happen if allergies affect the inner ear and balance.
- Drop in blood pressure during severe allergic reactions can also cause lightheadedness.
Do allergies cause back pain?
- Not directly, but constant sneezing and coughing can strain back muscles.
- Inflammation from allergies may worsen aches in sensitive individuals.
What does allergy acne look like?
- Allergy rashes may be mistaken for acne, but they differ:
- Allergy rash: itchy, red patches or hives that come and go quickly.
- Acne: pimples or blackheads that develop slowly and are often painful.
Can seasonal allergies cause itchy scalp?
Yes. Pollen can land on your hair and scalp, leading to itching.
- Washing your hair after outdoor activities helps reduce discomfort.
- Using gentle, fragrance-free shampoos can calm irritation.
10. Key Takeaways on Managing Allergy Rashes
Seasonal allergies aren’t just about sneezing and watery eyes—they can also affect your skin. Pollen exposure may lead to rashes, hives, and eczema flare-ups that make allergy season more uncomfortable.
- Most mild rashes improve with home care, antihistamines, and good skincare.
- Prevention is key: limit pollen exposure, wash regularly, and protect your skin barrier.
- See a doctor if symptoms are severe, persistent, or interfere with daily life.
- Emergency care is urgent for swelling of the throat, lips, or tongue, or if breathing becomes difficult.
👉 With the right mix of prevention, treatment, and medical support when needed, you can manage pollen allergy rashes and keep your skin healthier during allergy season.





